10-04-2017
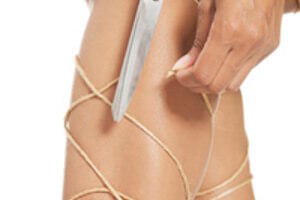
Sweet clover extract beneficial for oedema and lymphoedema
Standardised sweet clover extract is effective at relieving symptoms associated with lymphoedema and chronic venous insufficiency. Its main component, coumarin - a benzopyrone - is responsible for its anti-oedema effect. Since 1960, studies have demonstrated sweet clover extract’s benefits for patients suffering from venous insufficiency, varicose veins, thrombophlebitis, haemorrhoids, and lymphoedema of the lower limbs or following mastectomy.
Melilotus officinalis is mentioned in the French pharmacopaeia (1989) and in the botanical companion to the British pharmacopaeia (1996). Positive monographs on sweet clover-based preparations have been published by the European Scientific Cooperative on Phytotherapy (1997) as well as by the German Commission E on phytotherapeutic substances (March 1986, 1990).
Melilotus officinalis contains a wide range of coumarins, flavonoids and terpenoids. The dry extract, standardised to contain 18% coumarin, is obtained from its dried flowering tops.
Coumarin is a natural aromatic substance used in adjunct treatment of post-mastectomy lymphoedema alongside containment methods. It is a lactone (a benzopyrone), a cyclic ester, that was originally used as a seasoning. It is also found in tonka beans and lavender oil.
Different mechanisms of action
Used in the treatment of circulation problems related to lymphatic and venous function, standardised extract of melilotus officinalis may exert its effects act via different mechanisms of action:
The function of the lymphatic system is to drain the excess proteins and water which continually escape from the blood in small amounts, and to collect certain substances made in the tissues and any foreign bodies that enter it. The lymphatic system is comprised of small vessels that join together into larger ones. Lymphatic fluid is pumped into these vessels by the movements of adjacent muscles and by the contraction of the walls of the large lymphatic vessels. Finally, the lymphatic system empties into the blood circulation. Deficient function of the lymphatic system, including the drainage and return of interstitial fluid and proteins, can lead to the development of chronic damage associated with lymphoedema, a form of oedema with a high protein content.
Increases lymphatic circulation
In vitro studies on mesenteric vessels isolated from guinea pigs demonstrated a myotropic effect from a preparation containing an extract of melilotus officinalis, rutin and pure coumarin, that stimulated the rate and tone of the isolated lymphatic vessels 1.
In vivo, the same preparation led to a marked increase in lymphatic circulation in the thoracic duct of anaesthetised dogs2.
Its effects on accelerating lymphatic circulation have also been studied in dogs and in humans using lymphography. Intravenous administration to 10 volunteers of a melilotus-based preparation increased lymphatic circulation of the thoracic duct, confirming the lymphokinetic properties of this preparation and of coumarin3.
Treatment of lymphoedema
Lymphoedema is swelling of the arms or legs caused by the accumulation of lymphatic fluid in the interstitial spaces, mainly in subcutaneous fatty tissues, which results from a defect in the lymphatic system. It is characterised by an abnormal build-up of excess tissue proteins, with oedema, chronic inflammation and fibrosis.
There are three types of lymphoedema:
Benzopyrones like coumarin reduce all forms of oedema with a high protein content. They act by inciting macrophages to increase in number and by enhancing their normal lysis of excess proteins (the dissolution of lymphatic fluid proteins). Reducing excess protein diminishes fluid retention which in turn decreases oedema. This protein-reducing effect can be detected around four hours after administering a benzopyrone and peaks after 24 hours. The elimination of proteins and excess fluid begins within a few days although its effects are normally only apparent after six months, due to fibrous tissue.
Over a 12-week period, 25 women with lymphoedema of the arm, due to axillary lymphadenectomy for breast cancer, were given 20mg/day of sweet clover extract containing 20% coumarin. After six weeks, researchers noted a marked decrease in limb size. 4.
Another clinical study monitored 21 patients, four serving as a control group, 14 receiving a dry extract of sweet clover containing 8mg coumarin daily for six months, while three participants withdrew. The extract was shown to be effective at reducing lymphoedema in 11 subjects. The median reduction in upper arm circumference was around 5% compared with initial values5.
A meta-analysis reviewed 51 clinical studies conducted in eight countries which examined the effects of different benzopyrones, including coumarin, in treating lymphoedema. In all the studies, oral or topical use of benzopyrones produced a significant reduction in lymphoedema of between 40% and 71% within a year6. Symptoms, including infection, were similarly reduced in almost all the studies regardless of whether it was the arm or leg which was affected. Combining the 25 studies in which benzopyrone was administered orally, the average reduction in oedema over a year was 36% (1225 patients). Decreases were less marked in elephantiasis (-15% in a year) than for grades 1 and 2, because the oedema was obviously more serious to start with.
In 1993, three studies that looked at the use of coumarin in treating lymphoedema were published in Australia, India and China. Coumarin treatment reduced oedema volume in grade 2 lymphoedema of the arm by 2.2% per month (ie 40% in six months) and by 1.5% a month (ie 33% in six months) in grade 2 lymphoedema of the leg 7.
The significant swelling of those with elephantiasis decreased more rapidly but the overall reduction was smaller simply because the oedema was greater to begin with. While the reductions are slow, coumarin can thus transform what would otherwise be a disease that gradually (and sometimes rapidly) gets worse into one that slowly improves.
Venous insufficiency
An increase in capillary filtration and insufficiency of venous and lymphatic resorption are responsible for the development of oedema, one of the major symptoms associated with chronic venous insufficiency and varicose veins.
Sub-cutaneous injections of sweet clover extract and coumarin were shown to reduce formaldehyde-induced oedema in the hind legs of rats. The anti-oedema and anti-inflammatory properties of coumarin and sweet clover extract (12.5 to 100mg/kg i.p.) have been confirmed in several experimental models, such as kaolin-induced arthritis, thermal oedema and lymphostatic oedema 8 A sweet clover-based preparation significantly improved venous and lymphatic circulation in rabbits with venous stasis of the hind legs.
In two double-blind studies on a total of 414 patients with peripheral venous insufficiency, oral administration of a sweet clover-based preparation improved subjective symptoms (heaviness, pain, night cramps) and objective symptoms such as oedema9.
A comparative study was carried out on three groups of people : 20 received 200mg of a dry sweet clover extract a day, 15 were treated with ozone therapy and 20 with a combination of both treatments. The administration of the sweet clover extract for 15 days significantly reduced some of the symptoms of chronic venous insufficiency such as oedema, night cramps and heavy legs10. Studies involving a total of 1818 patients showed benefits from a sweet clover extract (standardised to 0.05% coumarin) combined with rutin in cases of venous insufficiency and phlebitis11, 12.
Improves blood circulation
Coumarin is responsible for the marked increase in blood circulation induced by taking a standardised extract of sweet clover.
Coumarin from sweet clover extract (5mg/kg given intravenously) was shown in dogs to increase capillary blood flow in organs and tissues such as the myocardium and striated muscle, and conferred a protective effect against ischaemic damage to the myocardium 13.
A study on dogs showed that a preparation containing a standardised extract of sweet clover, rutin and proxphyllin, administered intravenously for 1-4 weeks following coronary occlusion, was able to accelerate the development of collateral circulation and reduce histologic damage caused by ischaemia in myocardial tissue 14.
Pharmacokinetic
Pharmacokinetic studies on healthy volunteers show that orally-administered coumarin is rapidly and completely absorbed but that only between 2% and 6% of its free, intact form reaches the systemic circulation. This is due to extensive first-pass transformation (94-99%) into 7-hydroxycoumarin and its glucuronide.
The half-life of coumarin and 7-hydroxycoumarin is around one hour. Elimination of coumarin and its metabolites is mainly via urine.
---------------------------------------------------------------------------------
References :
1. Mislin H., Die Wirkung von cumarin aus melilotus officinalis auf di Funktion des Lymphangious Arzneim Forsch, Drug Resear, 21, 852-3 (1971).
2. Foldi M et al., Arztl Forsch. 16, 99 (1962).
3. Bartos V et al., Med. Klin., 65, 1701 (1970).
4. Muraca M.G. et al., I linfedemi degli arti superiori post-mastotectomia. Trattamiento con l'estratto di meliloto officinale, Gazz. Med. Ital., Arch. Sci. Med. 1999, 158: 133-6.
5. Patura G. et al., Linfedema dell arto superiore in pazinti operati per carcinoma della mamella esperienza clinica con estratto cumarinico Melilotus officinalis, Clin. Ter., 1999, 150: 403-8.
6. Casley-Smith J.R., Benzo-pyrones in the treatment of lymphoedema, 1999 March, vol. 16, N01: 31-41.
7. New England Journal of Medicine, 329 (1993), 1158-1163 ; Annals Tropical Medicine Parasitology (1993) 87, 247-258 ; British Medical Journal, 307 (1993) 1037-1040.
8. Földi-Börcsök E. et al., Die antiphlogistische une ödemhemmende Wirkung von cumarin au Melilotus officinalis, Arzneim Forsch., 21, 2025-30 (1971).
9. Borzeix M.G. et al., Arzneim Forsch., 45, 262 (1995).
10. Stefanini L. et al., Trattamento farmacologico e/o balneotherapico dell insufficienza venosa cronica, Gazz. Med. Ital., 1996, 155: 179-85.
11. Leng L.L. et al., Le traitement des varices au cours de la grossesse et dans le post partum. Expérimentation clinique de l'Esberiven, Bordeaux méd., 1974, 7 : 2755-6.
12. Babilliot, Contribution au traitement de l'insuffisance veineuse par Esberiven. Étude multicentrique sur 385 cas, Gaz. méd. fr., 1980, 87 : 3242-6.
13. Kovach A.G.B. et al., Arzneim Forsch., 20, 1630 (1970).
14. Sakai K. et al., Pharmacodyn. 242, 104 (1979).

Melilotus officinalis is mentioned in the French pharmacopaeia (1989) and in the botanical companion to the British pharmacopaeia (1996). Positive monographs on sweet clover-based preparations have been published by the European Scientific Cooperative on Phytotherapy (1997) as well as by the German Commission E on phytotherapeutic substances (March 1986, 1990).
Melilotus officinalis contains a wide range of coumarins, flavonoids and terpenoids. The dry extract, standardised to contain 18% coumarin, is obtained from its dried flowering tops.
Coumarin is a natural aromatic substance used in adjunct treatment of post-mastectomy lymphoedema alongside containment methods. It is a lactone (a benzopyrone), a cyclic ester, that was originally used as a seasoning. It is also found in tonka beans and lavender oil.
Different mechanisms of action
Used in the treatment of circulation problems related to lymphatic and venous function, standardised extract of melilotus officinalis may exert its effects act via different mechanisms of action:
- - lymphokinetic action relating to thoracic duct flow as demonstrated in volunteers;
- increased drainage of lymphatic fluid via direct stimulation of the lymphatic vessels;
- stimulation of macrophages increasing their phagocytoxic and proteolytic activity;
- improvement in quality and speed of the venous return;
- a capillary-protective effect.
The function of the lymphatic system is to drain the excess proteins and water which continually escape from the blood in small amounts, and to collect certain substances made in the tissues and any foreign bodies that enter it. The lymphatic system is comprised of small vessels that join together into larger ones. Lymphatic fluid is pumped into these vessels by the movements of adjacent muscles and by the contraction of the walls of the large lymphatic vessels. Finally, the lymphatic system empties into the blood circulation. Deficient function of the lymphatic system, including the drainage and return of interstitial fluid and proteins, can lead to the development of chronic damage associated with lymphoedema, a form of oedema with a high protein content.
Increases lymphatic circulation
In vitro studies on mesenteric vessels isolated from guinea pigs demonstrated a myotropic effect from a preparation containing an extract of melilotus officinalis, rutin and pure coumarin, that stimulated the rate and tone of the isolated lymphatic vessels 1.
In vivo, the same preparation led to a marked increase in lymphatic circulation in the thoracic duct of anaesthetised dogs2.
Its effects on accelerating lymphatic circulation have also been studied in dogs and in humans using lymphography. Intravenous administration to 10 volunteers of a melilotus-based preparation increased lymphatic circulation of the thoracic duct, confirming the lymphokinetic properties of this preparation and of coumarin3.
Treatment of lymphoedema
Lymphoedema is swelling of the arms or legs caused by the accumulation of lymphatic fluid in the interstitial spaces, mainly in subcutaneous fatty tissues, which results from a defect in the lymphatic system. It is characterised by an abnormal build-up of excess tissue proteins, with oedema, chronic inflammation and fibrosis.
There are three types of lymphoedema:
- grade 1 (spontaneously reversible): oedema is apparent when the skin is pressed, and decreases following elevation of the limb;
grade 2 (spontaneously irreversible): finger pressure no longer leaves a mark. Fibrosis has developed, marking the start of limb swelling and hardening of tissues. The oedema no longer responds to limb elevation;
grade 3 (lymphatic elephantiasis): at this stage, swelling is irreversible, the limb is typically very large and the tissue is hard (fibrotic)
Benzopyrones like coumarin reduce all forms of oedema with a high protein content. They act by inciting macrophages to increase in number and by enhancing their normal lysis of excess proteins (the dissolution of lymphatic fluid proteins). Reducing excess protein diminishes fluid retention which in turn decreases oedema. This protein-reducing effect can be detected around four hours after administering a benzopyrone and peaks after 24 hours. The elimination of proteins and excess fluid begins within a few days although its effects are normally only apparent after six months, due to fibrous tissue.
Over a 12-week period, 25 women with lymphoedema of the arm, due to axillary lymphadenectomy for breast cancer, were given 20mg/day of sweet clover extract containing 20% coumarin. After six weeks, researchers noted a marked decrease in limb size. 4.
Another clinical study monitored 21 patients, four serving as a control group, 14 receiving a dry extract of sweet clover containing 8mg coumarin daily for six months, while three participants withdrew. The extract was shown to be effective at reducing lymphoedema in 11 subjects. The median reduction in upper arm circumference was around 5% compared with initial values5.
A meta-analysis reviewed 51 clinical studies conducted in eight countries which examined the effects of different benzopyrones, including coumarin, in treating lymphoedema. In all the studies, oral or topical use of benzopyrones produced a significant reduction in lymphoedema of between 40% and 71% within a year6. Symptoms, including infection, were similarly reduced in almost all the studies regardless of whether it was the arm or leg which was affected. Combining the 25 studies in which benzopyrone was administered orally, the average reduction in oedema over a year was 36% (1225 patients). Decreases were less marked in elephantiasis (-15% in a year) than for grades 1 and 2, because the oedema was obviously more serious to start with.
In 1993, three studies that looked at the use of coumarin in treating lymphoedema were published in Australia, India and China. Coumarin treatment reduced oedema volume in grade 2 lymphoedema of the arm by 2.2% per month (ie 40% in six months) and by 1.5% a month (ie 33% in six months) in grade 2 lymphoedema of the leg 7.
The significant swelling of those with elephantiasis decreased more rapidly but the overall reduction was smaller simply because the oedema was greater to begin with. While the reductions are slow, coumarin can thus transform what would otherwise be a disease that gradually (and sometimes rapidly) gets worse into one that slowly improves.
Venous insufficiency
An increase in capillary filtration and insufficiency of venous and lymphatic resorption are responsible for the development of oedema, one of the major symptoms associated with chronic venous insufficiency and varicose veins.
Sub-cutaneous injections of sweet clover extract and coumarin were shown to reduce formaldehyde-induced oedema in the hind legs of rats. The anti-oedema and anti-inflammatory properties of coumarin and sweet clover extract (12.5 to 100mg/kg i.p.) have been confirmed in several experimental models, such as kaolin-induced arthritis, thermal oedema and lymphostatic oedema 8 A sweet clover-based preparation significantly improved venous and lymphatic circulation in rabbits with venous stasis of the hind legs.
In two double-blind studies on a total of 414 patients with peripheral venous insufficiency, oral administration of a sweet clover-based preparation improved subjective symptoms (heaviness, pain, night cramps) and objective symptoms such as oedema9.
A comparative study was carried out on three groups of people : 20 received 200mg of a dry sweet clover extract a day, 15 were treated with ozone therapy and 20 with a combination of both treatments. The administration of the sweet clover extract for 15 days significantly reduced some of the symptoms of chronic venous insufficiency such as oedema, night cramps and heavy legs10. Studies involving a total of 1818 patients showed benefits from a sweet clover extract (standardised to 0.05% coumarin) combined with rutin in cases of venous insufficiency and phlebitis11, 12.
Improves blood circulation
Coumarin is responsible for the marked increase in blood circulation induced by taking a standardised extract of sweet clover.
Coumarin from sweet clover extract (5mg/kg given intravenously) was shown in dogs to increase capillary blood flow in organs and tissues such as the myocardium and striated muscle, and conferred a protective effect against ischaemic damage to the myocardium 13.
A study on dogs showed that a preparation containing a standardised extract of sweet clover, rutin and proxphyllin, administered intravenously for 1-4 weeks following coronary occlusion, was able to accelerate the development of collateral circulation and reduce histologic damage caused by ischaemia in myocardial tissue 14.
Pharmacokinetic
Pharmacokinetic studies on healthy volunteers show that orally-administered coumarin is rapidly and completely absorbed but that only between 2% and 6% of its free, intact form reaches the systemic circulation. This is due to extensive first-pass transformation (94-99%) into 7-hydroxycoumarin and its glucuronide.
The half-life of coumarin and 7-hydroxycoumarin is around one hour. Elimination of coumarin and its metabolites is mainly via urine.
---------------------------------------------------------------------------------
References :
1. Mislin H., Die Wirkung von cumarin aus melilotus officinalis auf di Funktion des Lymphangious Arzneim Forsch, Drug Resear, 21, 852-3 (1971).
2. Foldi M et al., Arztl Forsch. 16, 99 (1962).
3. Bartos V et al., Med. Klin., 65, 1701 (1970).
4. Muraca M.G. et al., I linfedemi degli arti superiori post-mastotectomia. Trattamiento con l'estratto di meliloto officinale, Gazz. Med. Ital., Arch. Sci. Med. 1999, 158: 133-6.
5. Patura G. et al., Linfedema dell arto superiore in pazinti operati per carcinoma della mamella esperienza clinica con estratto cumarinico Melilotus officinalis, Clin. Ter., 1999, 150: 403-8.
6. Casley-Smith J.R., Benzo-pyrones in the treatment of lymphoedema, 1999 March, vol. 16, N01: 31-41.
7. New England Journal of Medicine, 329 (1993), 1158-1163 ; Annals Tropical Medicine Parasitology (1993) 87, 247-258 ; British Medical Journal, 307 (1993) 1037-1040.
8. Földi-Börcsök E. et al., Die antiphlogistische une ödemhemmende Wirkung von cumarin au Melilotus officinalis, Arzneim Forsch., 21, 2025-30 (1971).
9. Borzeix M.G. et al., Arzneim Forsch., 45, 262 (1995).
10. Stefanini L. et al., Trattamento farmacologico e/o balneotherapico dell insufficienza venosa cronica, Gazz. Med. Ital., 1996, 155: 179-85.
11. Leng L.L. et al., Le traitement des varices au cours de la grossesse et dans le post partum. Expérimentation clinique de l'Esberiven, Bordeaux méd., 1974, 7 : 2755-6.
12. Babilliot, Contribution au traitement de l'insuffisance veineuse par Esberiven. Étude multicentrique sur 385 cas, Gaz. méd. fr., 1980, 87 : 3242-6.
13. Kovach A.G.B. et al., Arzneim Forsch., 20, 1630 (1970).
14. Sakai K. et al., Pharmacodyn. 242, 104 (1979).
Order the nutrient mentioned in this article
Further reading
24-08-2016
Almost 600 studies - the majority conducted in Russia - have been published on the effects of taxifolin, a powerful flavonoid extracted from Siberian larch....
Read more31-07-2019
Although summertime may be conducive to rest and relaxation, the hot weather can significantly exacerbate the sensation of heavy legs. When temperatures start to rise,...
Read more19-05-2015
30% of the population suffer from venous insufficiency – four times as many women as men. To prevent this chronic, progressive disease from getting worse,...
Read more© 1997-2026 Fondation pour le Libre Choix
All rights reserved
All rights reserved
Free
Thank you for visiting our site. Before you go
REGISTER WITHClub SuperSmart
And take advantage
of exclusive benefits:
of exclusive benefits:
- Free: our weekly science-based newsletter "Nutranews"
- Special offers for club members only