Keeping your teeth for life: the secrets and nutritional tips you need to know

There are many things we like to put off till the next day, but for some strange reason, taking care of our teeth seems to be one of the most common. While we’re happy to spend hours looking after our hair, skin and even eyes, we barely devote two minutes a day to our teeth and ignore all the micronutrients that can help maintain them in tip-top condition …
If you were asked to list the nutritional factors that prevent tooth loss, you might mention calcium and a low-sugar diet, but would you able to think of anything else?
Sadly, our ignorance soon comes back to haunt us: on average, we lose four teeth between the ages of 45 and 55 (1). And after that, everything speeds up: the figure rises to 10 teeth over the following decade, with 15%-30% of Western populations having lost all their teeth after their mid-sixties.
But by discovering the nutritional mechanisms that help prevent tooth loss, you could keep your teeth for an extra ten years or so, and even hold on to them into very old age. According to the WHO, dental infections resulting in tooth loss are among the chronic diseases that could be avoided through good nutrition (2).
Losing your teeth: a distressing experience with more serious consequences than you might think
We always under-estimate the importance of our teeth. It’s only when we lose our first tooth that we realise just how crucial they are.
First of all, there’s our smile, that tool of seduction we use to express pleasure, satisfaction and well-being. Looking at ourselves in the mirror, we immediately see the extent of the damage: “My god, my smile is ruined … it completely changes my face! I don’t recognise myself … ”. This awful realisation is very often accompanied by a loss of self-confidence, and feelings of self-contempt and even shame. “What will people think? They’ll say I don’t take proper care of myself, that I’ve let myself go”.
The negative psychological effects, which no medication can mitigate, will only get worse, especially as things aren’t going to get any easier. If a tooth has fallen out prematurely, there’s every chance that other teeth will soon follow. The way others look at you becomes hard to bear. When you’re missing certain teeth, the lips lose support, causing a gradual collapse of the lower part of the face. Facial expressions change completely (3).
Unfortunately, losing teeth doesn’t just cause aesthetic problems. It also significantly increases the risk of several diseases. A trawl through the scientific literature reveals the following:
- a shorter lifespan associated with premature tooth loss;
- a higher risk of cardiovascular disease (4), and in particular, of hypertension (5) from the moment the first teeth are lost;
- impairment of certain sensory functions (especially reaction times and auditory function) (6);
- acceleration of cognitive decline (7) (several studies show that memory and speed of information-processing decline faster in people who have lost their teeth).
- a reduction in physical ability;
- an increased risk of three forms of cancer: of the oesophagus (136% additional risk), neck (68%) and lungs (54%).
These health risks are in addition to the many constraints posed by wearing removable dentures or ‘false teeth’, the primary cause of bad breath in those over 50.
Tooth loss: what are the real causes?
When you lose a tooth for the first time, it’s often when you’re doing something ordinary, like eating an apple or a piece of bread, for example. It’s usually a molar or a premolar (canines are the teeth we keep the longest (8-10)). But what’s the real reason for this tooth loss?
In fact, there are just four causes and they overlap:
- Dental caries (in almost 60% of cases) (11).
- Periodontitis (in 20-30 % of cases). Periodontitis is an inflammatory disease affecting the gums and bones around the teeth: pathogenic bacteria accumulate in the junction between tooth and gum causing disease which gradually damages the tooth’s supporting tissues.
- Mal-positioned teeth (hence the importance of orthodontics);
- Impact and trauma.
“I tell thee, Sancho, a mouth without teeth is like a mill without a millstone, and a tooth is much more to be prized than a diamond;”, Cervantes’ Don Quixote
So what makes us get dental caries and periodontitis, the two main causes of tooth loss?
These two dental problems develop slowly. Throughout life, in fact.
Our mouths are host to billions of microorganisms from more than 1000 different species, most of which are beneficial for our health. Some float around in the oral milieu, some thrive on the tongue, while others stick to our teeth. Immediately after brushing, proteins in our saliva adhere to the tooth wall (this is the salivary biofilm) and attract harmless colonising bacteria. After a few minutes, they’re joined by other bacteria, forming a complex habitat around which develops an increasingly strong barrier: dental plaque.
This plaque, which is constantly being added to by bacterial secretion products, poses no threat as long as the microorganisms developing in it are beneficial. Unfortunately, when we eat foods high in carbohydrates, particularly simple ones like sucrose, we encourage the growth of pathogenic bacteria within this plaque.
These bacteria are attracted by the plaque’s sugary residues. They use it to produce vast carbohydrate chains, recruiting huge numbers of other similar bacteria. They then feed on these sugars and release lactic acid, a compound which is toxic to other bacteria and particularly harmful for the teeth.
There’s nothing as good as thorough brushing for getting rid of this unwelcome little community. It dislodges pathogenic bacteria from the teeth and removes the particles of sugary food that feed their growth. But it’s not enough. When we eat pasta for lunch (which is high in complex carbohydrates) or have a fizzy drink in the early afternoon (very high in sucrose), it’s likely that another eight hours will pass before our toothbrushes have the opportunity to remove the pathogenic bacteria that have accumulated.
So in the intervening period, they have plenty of time to break down the sugars and release acid. If the acidity in contact with the teeth falls below the critical pH of 5.5, tooth enamel starts to deteriorate. This happens frequently, particularly if you snack between meals. Bedtime brushing interrupts this deterioration but it will inevitably start again the next day! It’s as if you have a team of workers digging a hole in your tooth who each morning tirelessly pick up where they left off the day before. This deterioration normally occurs in areas of the mouth that are difficult for the tongue and saliva to reach, such as the molars. The speed and intensity of this hole-digging depends on your diet and lifestyle. The higher your sugar intake, the bigger the team of diggers and the faster the hole will appear. If your mineral intake is less than optimal, the enamel will be less resistant and bacteria will find it easier to break through.
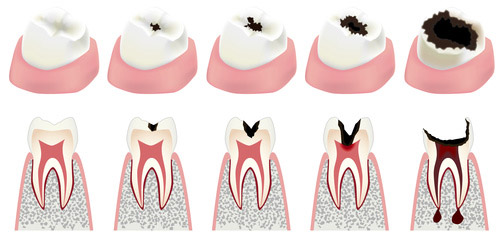
Then one day, after working for several months, years or even decades, the diggers reach the tooth’s dentine. This is found beneath the enamel, the tooth’s protective layer. From here on in, things move fast. Less mineralised than enamel, dentine is much less resistant to acidity: if the pH falls below 6.2, dentine will break down too. This means that from now on, you will not be able to tolerate the same intake of sugar as before. If a 60 year-old whose enamel has been ‘breached’ drinks a sugary drink, the consequences will be much greater than they would for someone in their 20s.
Thereafter, the hole in the tooth continues to get deeper, forming an actual tunnel, through which the pathogenic bacteria finally reach the tooth’s pulp at which point the dental caries becomes particularly painful. But even that’s not the end of it: if nothing is done, the bacteria can go on to attack the ligament, bone or gum, and even get into the bloodstream! And the tooth is hanging on by a thread …
So to prevent this process, we need to brush our teeth more often, right?
You might assume that brushing your teeth more often, say every hour, would be the right approach to preventing bacterial plaque from forming all the time. But in fact, it’s not: over the long term, excessive brushing damages the tooth’s surface and actually encourages tooth decay. L'Union Française pour la Santé Bucco-Dentaire (the French Union for Oral Health) thus recommends brushing twice a day, once in the morning and once at night, no more.
In fact, it’s best to tackle the problem with one of our natural weapons: saliva. We only realise how essential it is when the saliva glands are affected by disease or in the course of ageing. Saliva offers many benefits for combatting pathogenic bacteria:
- it reduces the contact time between the tooth’s surface and sugar;
- it contains the enzyme lactoperoxidase, a natural anti-bacterial agent;
- it contains lactoferrin which inhibits the metabolism of iron necessary for bacteria to grow;
- it makes the environment less acid - pathogenic bacteria prefer acidity.
If older people suffer more with dental caries, it’s also because saliva production decreases as we age. The same is true for smokers.
There are two ways of making the best use of this natural weapon:
- Avoid eating a processed diet, with softer foods, as it significantly reduces mastication and saliva secretion and also contains far too many acidifying liquid foods such as soft drinks (which prevent saliva from effectively lowering the mouth’s acidity).
- Start chewing gum again (avoiding the sugar-loaded varieties): there’s nothing more effective than chewing gum for stimulating salivation without ingesting calories. Though a lot of people aren’t aware of it, this is one of the recommendations made by numerous oral health organisations and associations.
When we brush our teeth, we eliminate all bacteria, including the beneficial kind. By stimulating the flow of saliva, chewing gum helps get rid of just the ‘bad’ bacteria, the ones that thrive in an acid environment.
Oral probiotics, an emerging field, offer the same advantage.
These beneficial bacteria, primarily from the strains Lactobacillus and Bifidobacterium, are able to check the growth of the pathogenic microorganisms responsible for tooth decay (12).
Though they come in a freeze-dried form, they’re actually still ‘live’: once reintroduced into a soluble milieu like the mouth, they leave their dormant state and become active again. In order to colonise the environment and combat pathogenic bacteria, probiotics require nourishment from a specific food called fructooligosaccharides. Unlike simple sugars, these compounds act like soluble fibre in the body and as a result, are not converted by pathogenic bacteria. They are thus added to oral probiotic supplements to provide support to the ‘friendly’ bacteria, enabling them to compete with their ‘unfriendly’ counterparts.
If you plan to try this ground-breaking new option, don’t be fooled by appearances: rest assured that fructooligosaccharides are recognised as beneficial for health and have nothing to do with the sucrose responsible for dental caries. Even our taste buds can be taken in by them!
Micronutrients that boost the efficacy of your saliva
Saliva is a powerful weapon provided it has optimal composition. As this depends mainly on diet, it’s no surprise that deficiency in several micronutrients accelerates the process of tooth loss and disrupts the tooth remineralisation process (13).
The most important of these micronutrients is vitamin D.
We’ve known for decades that vitamin D maintains the structure of the skeleton, helps keep our bones and kidneys healthy, reduces the risk of cardiovascular disease, combats inflammation and stimulates the immune system (14). More recently though, we’ve learned that it also significantly influences oral health. This is as a result of several actions:
- Regulation of the calcium-phosphate balance: it increases absorption of calcium and phosphate (two minerals essential for enamel) from the gastrointestinal tract, as well as reabsorption of calcium in the kidneys (which promotes remineralisation of the teeth).
- Immune-modulating effects: it increases the mechanisms of innate and acquired immune response that intervene against oral bacteria.
- An anti-infectious effect: it plays a role in the production of antimicrobial peptides.
- Intervention in sugar metabolism: it promotes the conversion of proinsulin into insulin.
A number of studies have thus shown that adequate vitamin D levels may help combat the development of periodontitis (affecting the tooth bone), one of the two causes of tooth loss. Vitamin D may prevent generation of the pro-inflammatory cytokines IL-1b and TNF-α both of which play a key role in the pathogenesis of periodontitis by causing bone resorption (destruction of bone tissue) and by impairing the healing process (15-16). A number of studies have also identified a link between a low intake of vitamin D (less than 800IU a day) and the presence of periodontal disease markers (17-19). Conversely, supplementation helps reduce loss of alveolar bone as well as TNF-α levels in the gums (20).
br>But that’s not all - vitamin D is also effective when it comes to dental caries! Several studies have shown an association between low levels of circulating vitamin D and a higher risk of dental caries (21). Researchers have found, for example, that children with no tooth decay were two to three times more likely to have optimal vitamin D levels. It’s a similar story when it comes to endogenous production of vitamin D from the sun: in the United States, the sunnier the region, the greater the vitamin D production and the lower the prevalence of dental caries (22).
A meta-analysis of 24 clinical trials recently confirmed these observations, demonstrating that vitamin D supplementation helped prevent dental caries (23). Other research has shown that almost all people who live at high or middle latitudes have inadequate vitamin D levels between the months of October and April.
Calcium is also a crucial micronutrient.
Epidemiological studies suggest it may prevent both dental caries and periodontitis (28-30). And there’s a clear explanation for this: the presence of calcium and phosphate in bacterial plaque and in saliva increases the remineralisation of enamel and reduces the adherence of bacteria associated with tooth decay (31-32).
Other factors highlighted by the scientific community:
- Low levels of vitamin B12, which are increasingly common, are also associated with increased incidence of periodontitis and tooth loss (33).
- The type of fat you consume is also important: too much omega-6 in relation to omega-3 accelerates the progress of periodontal disease (34).
- Vitamins B6 (35), K (36) and C also act against dental caries.
- The gums are among the areas of the body with the highest rate of tissue replacement and protein is a key element for ensuring this replacement takes place effectively.
In summary, if you want to hold on to your teeth for as long as possible, follow these eight recommendations:
- Chew gum every day, especially after lunch (opt for sugar-free and the most natural form possible) ;
- Ensure you have an adequate intake of vitamin D by taking supplements, at least in autumn and winter when circulating levels are at their lowest, and by getting a reasonable amount of sun exposure in the spring and summer.
- Make sure your calcium intake is adequate, by increasing your consumption of calcium-rich foods and considering supplementation.
- Brush your teeth twice a day, but avoid using an electric toothbrush as they are more abrasive and may damage tooth enamel in the long term (37).
- Eat fresh fruits and vegetables and studiously avoid fizzy drinks, processed foods and high-sugar foods.
- Take oral probiotics such as Oral Health especially if you feel you’re lacking in saliva, are over 60 or are a smoker, to restore optimal bacterial equilibrium in your mouth and to combat pathogenic bacteria.
- Take a multivitamin every day such as Daily 3 to prevent deficiency in certain micronutrients.
- Drink at least two litres of water a day.
Don’t for a minute believe that losing your teeth is a normal part of ageing! In almost all cases, tooth loss is not directly linked to the ageing process but to the development of pathogenic bacteria.
References
- Nitschke I, Hopfenmüller W: Die Zahnmedizinische Versorgung älterer Menschen. [Dental care for older people.] In: Mayer, K. U. and Baltes, P. B.: Die Berliner Altersstudie. [The Berlin Aging Study.] Berlin: Akademie Verlag: 429–448; ISBN-13: 978-3050045085 (1996)
- Touger-Decker R, Mobley C (2013) Academy of nutrition and dietetics. Position of the academy of nutrition and dietetics: oral health and nutrition. J Acad Nutr Diet 113:693–701
- POUYSSEGUR Valérie, et al. Impact de la détérioration buccale sur le processus de vieillissement » Unité Odontologie Gériatrique CHU Nice. Le Chirurgien-dentiste de France, 17111/2005, n°1233, pp150-158
- Lowe G., Woodward M., Rumley A., Morrison C., Tunstal-Pedoe H. & Stephen K. (2003) Total tooth loss and prevalent cardiovascular disease in men and women: possible roles of citrus fruit consumption, vitamin C, and inflammatory and thrombotic variables. Journal of Clinical Epidemiology 56:694-700.
- Joshua H Gordon, Michael J LaMonte, Jiwei Zhao, Robert J Genco, Thomas R Cimato, Kathleen M Hovey, Matthew A Allison, Charles P Mouton, Jean Wactawski-Wende. Association of Periodontal Disease and Edentulism With Hypertension Risk in Postmenopausal Women. American Journal of Hypertension, 2018; DOI: 10.1093/ajh/hpy164
- Osterberg T., Era P., Gause-Nilsson I. & Steen B. (1995) Dental state and functional capacity in 75-year-olds in three Nordic localities. Journal of Oral Rehabilitation 22:653-660.
- D. Cerutti-Kopplin, J. Feine, D. M. Padilha, R. F. de Souza, M. Ahmadi, P. Rompre, L. Booij, E. Emami. Tooth Loss Increases the Risk of Diminished Cognitive Function: A Systematic Review and Meta-analysis. JDR Clinical & Translational Research, 2016; 1 (1): 10 DOI: 10.1177/2380084416633102
- Battistuzzi P., Kayser A. & Peer P. (1987) Tooth loss and remaining occlusion in a Dutch population. Journal of Oral Rehabilitation 14:541-547.
- Papapanou P.N., Wennstrom J.L. & Grondahl K. (1989) A 10-year retrospective study of periodontal disease progression. Journal of Clinical Periodontology 16:403-411.
- Paulander J., Axelsson P., Lindhe J.& Wennstrom J. (2004) Intra-oral pattern of tooth and periodontal bone loss between the age of 50 and 60 years. A longitudinal prospective study. Acta Odontologica Scandinavica 62:214-222.
- Richards W., Ameen J., Coll A.M. & Higgs G. (2005) Reasons for tooth extraction in four general dental practices in South Wales. British Dental Journal 198:275-278.
- Meurman JH. Probiotics: do they have a role in oral medicine and dentistry? Eur J Oral Sci. 2005;113:188-96.
- Alvarez, J. O. (1995) Nutrition, tooth development, and dental caries. American Journal of Clinical Nutrition 61, 410S–416S
- Christakos S, Dhawan P, Verstuyf A, Verlinden L, Carmeliet G. Vitamin D: metabolism, molecular mechanism of action, and pleiotropic effects. Physiological Reviews 2016; 96 (1): 365–408. doi: 10.1152/physrev.00014.2015 [PMC free article] [PubMed]
- Jimenez M, Giovannucci E, Krall Kaye E et al (2014) Predicted vitamin D status incidence of tooth loss and periodontitis. Public Health Nutr 17:844–852
- Stein SH, Livada R, Tipton DA (2014) Re-evaluating the role of vitamin D in the periodontium. J Periodont Res 49:545–553
- Alshouibi EN, Kaye EK, Cabral HJ et al (2013) Vitamin D and periodontal health in older men. J Dent Res 92:689–693
- Dietrich T, Joshipura KJ, Dawson-Hughes B et al (2004) Association between serum concentrations of 25-hydroxy vitamin D3 and periodontal disease in the US population. Am J Clin Nutr 80:108–113
- Miley DD, Garcia MN, Hildebolt CF et al (2009) Cross-sectional study of vitamin D and calcium supplementation effects in chronic periodontitis. J Periodontol 80:1433–1439
- Wang Q, Li H, Xie H et al (2013a) 25-hydroxy vitamin D3 attenuates experimental periodontitis through downregulation of TLR4 and JAK1/STAT3 signaling in diabetic mice. J Steroid Biochem Mol Biol 135:43–50
- Schroth RJ, Levi JA, Sellers EA et al (2013) Vitamin D status of children with severe early childhood caries: a case–control study. BMC Pediatr 13:174
- Grant WB (2011) A review of the role of solar ultraviolet-B irradiance and vitamin D in reducing risk of dental caries. Dermatoendocrinol 3:193–198
- Hujoel PP (2013) Vitamin D and dental caries in controlled clinical trials: systemic review and meta-analysis. Nutr Rev 71:88–97
- Ganji V, Zhang X, Tangpricha V. Serum 25-hydroxyvitamin D concentrations and prevalence estimates of hypovitaminosis D in the U.S. population based on assay-adjusted data. J Nutr 2012;142(3):498–507. doi: 10.3945/jn.111.151977
- Greene-Finestone LS, Berger C, de Groh M, Hanley DA, Hidiroglou N, Sarafin K et al. 25-Hydroxyvitamin D in Canadian adults: biological, environmental, and behavioral correlates. Osteoporos Int2011;22(5):1389–1399. doi: 10.1007/s00198-010-1362-7
- Płudowski P. Konstantynowicz J, Jaworski K. Assessment of vitamin D status in Polish adult population. Standardy Medyczne/Pediatria 2014;(11):609–617.
- Vierucci F, Del Pistoia M, Fanos M, Erba P, Saggese G. Prevalence of hypovitaminosis D and predictors of vitamin D status in Italian healthy adolescents. It J Pediatr 2014;40:54 doi: 10.1186/1824-7288-40-54
- Adegboye ARA, Twetman S, Christensen LB, Heitmann BL (2012) Intake of dairy calcium and tooth loss among adult Danish men and women. Nutrition 28:779–784
- Hung HC, Willett W, Ascherio A, Rosner BA, Rimm E, Joshipura KJ (2003) Tooth loss and dietary intake. J Am Dent Assoc 134:1185– 1192
- Adegboye AR, Fiehn NE, Twetman S, Christensen LB, Heitmann BL (2010) Low calcium intake is related to increased risk of tooth loss in men. J Nutr 140:1864–1868
- Moynihan P, Petersen PE (2004) Diet, nutrition and the prevention of dental diseases. Public Health Nutr 7:201–226
- Danielsson NL, Hernell O, Johansson I (2009) Human milk compounds inhibiting adhesion of mutans streptococci to host ligandcoated hydroxyapatite in vitro. Caries Res 43:171–178
- Zong, G., Holtfreter, B., Scott, A. E., Volzke, H., € Petersmann, A., Dietrich, T., Newson, R. S. & Kocher, T. (2016) Serum vitamin B12 is inversely associated with periodontal progression and risk of tooth loss: a prospective cohort study. Journal of Clinical Periodontology 43, 2–9.
- Iwasaki, M., Taylor, G. W., Moynihan, P., Yoshihara, A., Muramatsu, K., Watanabe, R. & Miyazaki, H. (2011) Dietary ratio of n-6 to n-3 polyunsaturated fatty acids and periodontal disease in community-based older Japanese: a 3-year follow-up study. Prostaglandins, Leukotrienes and Essential Fatty Acids 85, 107–112.
- Salam, R. A., Zuberi, N. F. & Bhutta, Z. A. (2015) Pyridoxine (vitamin B6) supplementation during pregnancy or labour for maternal and neonatal outcomes. The Cochrane Database of Systematic Reviews 6, CD000179.
- Southward, K. (2015) A hypothetical role for vitamin K2 in the endocrine and exocrine aspects of dental caries. Medical Hypotheses 84, 276–280
- Bizhang M, Schmidt I, Chun Y-HP, Arnold WH, Zimmer S (2017) Toothbrush abrasivity in a long-term simulation on human dentin depends on brushing mode and bristle arrangement. PLoS ONE 12(2): e0172060. doi.org/10.1371/journal.pone.0172060

Sugar- and aspartame-free chewing gum with essential oil of Pistacia lentiscus
www.supersmart.comAll rights reserved
Free
Thank you for visiting our site. Before you go
REGISTER WITHClub SuperSmart
of exclusive benefits:
- Free: our weekly science-based newsletter "Nutranews"
- Special offers for club members only