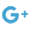Diabetes in complete remission following several months’ treatment with a natural substance
 “There’s no cure for diabetes. It’s a chronic disease for which lifelong medication is necessary.” You’ve probably heard this a thousand times, but from now on, it can be refuted. A new study has just shown that significant weight loss (more than 10kg) can reverse the processes involved in type 2 diabetes and put the condition into remission.
“There’s no cure for diabetes. It’s a chronic disease for which lifelong medication is necessary.” You’ve probably heard this a thousand times, but from now on, it can be refuted. A new study has just shown that significant weight loss (more than 10kg) can reverse the processes involved in type 2 diabetes and put the condition into remission.
This has sent shock waves across the medical world. Until very recently, it was thought that the loss of insulin sensitivity in fat cells and the failure of beta-pancreatic cells which occurs in type 2 diabetes was irreversible. But the large-scale Diabetes Remission Clinical Trial (DiRECT) has just put paid to this assumption: over half the type 2 diabetics who participated were able to revert to a long-term non-diabetic state after losing a significant amount of weight and maintaining it for at least 12 months.
To achieve this, they obviously had to follow a low-calorie diet, learn to eat more healthily and reduce their blood sugar levels naturally. They quickly saw a decrease in the fat content of their liver and pancreas (two signs of diabetes) though it took several months before their beta-pancreatic cells were restored to their original condition and they regained normal insulin sensitivity.
How were these individuals able to conquer their diabetes?
Eating a meal or a snack produces a huge influx of different nutrients into the body, all of which serve as fuel for our cells. Without these nutrients, our cells wouldn’t survive for very long: they draw on them for energy in order to fulfil their physiological functions. But this energy supply needs to be constant, with the slightest shortage proving fatal! If we take the example of a washing machine, it can only work as long as it has an electricity supply. If you unplug the lead, you immediately cut off the energy supply and the machine stops. This is similar to what would happen to cells if their energy supply were interrupted – but with one small difference. When you plug the washing machine back in, it starts to work normally again, while a cell deprived of energy for too long will never come back to life.
The body has thus come up with a regulatory system to enable a consistent amount of fuel to be supplied to cells via the bloodstream. It’s a well-honed system which stabilises the amount of glucose in the blood. Why glucose? Because it’s one of the most energy-rich nutrients and because digestive enzymes convert numerous large molecules into glucose.
When there’s a rise in blood glucose levels, for example after a meal, a group of cells in the pancreas (beta-pancreatic cells) release a substance which orders the glucose to be absorbed into muscle and fat cells, thus restoring normal blood sugar levels. This substance isinsulin. The sugar, stored in the form of fat or glycogen, will be reintroduced into the bloodstream later, as required.
In type 2 diabetics, this system becomes progressively defective. Initially, it’s probably caused by a diet-related problem. When food intake is too rich or unbalanced, it results in regular spikes in blood sugar. The body reacts, as it’s supposed to, by releasing huge amounts of insulin which leads to excess sugar being stored in the form of fat. It’s not a problem if these unhealthy dietary choices are made occasionally, but if it happens repeatedly, it’s not long before adverse changes start to occur. Slowly but surely, fat cells expand like balloons, pushing the needle on the bathroom scales higher and higher. Before long, these superfluous reserves start to become a problem, especially around the abdomen. This would normally encourage people to get their weight back under control as soon as possible, but if they choose to ignore it, diabetes will start to develop.
As the fat cells grow bigger, they refuse to admit new energy reserves. No longer compliant, they gradually become what’s called ‘insulin-resistant’. The inevitable outcome is that sugar which would normally be stored in reserve cells remains in the bloodstream, which obviously leads to an increase in blood sugar levels. In such cases, individuals are described as being chronically hyperglycaemic. It’s a dangerous situation which can lead to progressive deterioration of the nerves, blood vessels, eyes and kidneys. What’s more, the risks are so great that the body starts to quickly establish a defence strategy: beta-pancreatic cells are forced to release yet more insulin from the pancreas. As the fat cells are no longer ‘playing ball’, they’re confronted with even greater amounts of insulin. It’s a fitting strategy but it has to be constantly readjusted to compensate for the increasing insulin-resistance of the fat cells. Thus the resistance borders on insurrection. Ensuring the sugar is stored in cells and acceptable blood sugar levels are maintained requires the release of astronomical amounts of insulin and a frenetic and unsustainable rate of production by the beta-pancreatic cells. It’s hardly surprising then, that after a while, they give up. Beta cells that have survived high blood glucose levels gradually lose their ability to secrete insulin. This is a dramatic development since insulin is the only hormone in the body that can reduce glycaemia. Without it, blood sugar levels become very unstable, resulting in potentially serious health problems.
It is this inability to produce normal amounts of insulin that was hitherto thought to be irreversible. But the findings of this study are conclusive: provided an individual’s diabetes has been present for less than 10 years, the beta-pancreatic cells can re-learn to produce insulin and become ‘normal’ again. But for that to happen, the factors that led to the original failure of the beta-pancreatic cells must be dealt with. In other words, action must be taken to address the three main mechanisms involved in the development of diabetes:
- An unhealthy diet that leads to weight gain.
- Excess weight that causes cells to become insulin-resistant.
- Insulin-resistance which first leads to an increase in insulin production, and then a gradual decrease as beta-pancreatic cells stop secreting insulin.
So how can we respond quickly to combat diabetes naturally?
The study shows that it’s possible to overcome diabetes provided you don’t wait too long to act: after more than 10 years with the condition, it appears that beta-pancreatic cells have been too deeply-affected to recover and return to normal production of adequate insulin levels.
To put diabetes into remission, there are three essential steps that need to be followed:
- Take action against excess weight, particularly in the abdominal area, to improve insulin-resistance.
- Take action against glycaemia to stop beta-pancreatic cells getting ‘burned out’.
- Take action against the complications of diabetes to prevent the development of new health problems.
Over the years, scientists have endeavoured to find a drug that could act on all three fronts at the same time. There have been times when they believed they’d succeeded but each of the medications introduced proved unsuitable for certain people or caused significant side-effects. Recently, focus has switched to a natural product called berberine. This is a substance extracted from barberry, a shrub that grows to around 2-3 metres high and which has been traditionally used for thousands of years to ‘purify the blood’ and treat inflammatory disorders. It seems that once again, the scientific community is looking to traditional medicine to provide solutions. And once again, they’re right to do so.
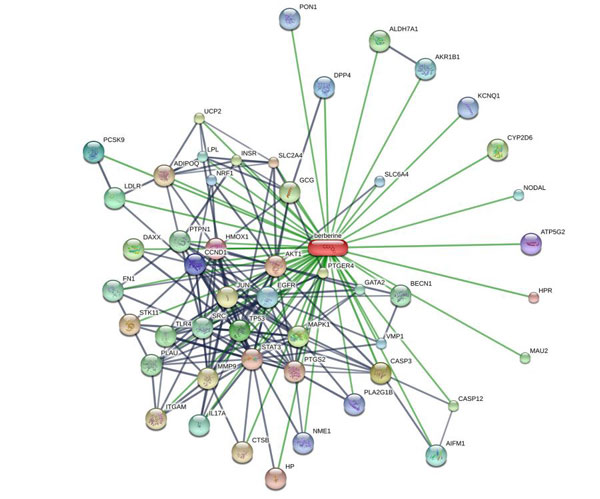
Recent studies have shown that berberine is an ideal candidate for treating diabetes. It offers exceptional benefits in terms of lowering levels of blood glucose and blood cholesterol and supporting weight control (2-5). The only reason it’s not well-known is because its precise mechanism of action has yet to be identified. Unlike drugs, it seems to be able to influence numerous mechanisms associated with blood glucose, lipogenesis (the process whereby fat cells store energy) and insulin-sensitivity. The diagram below shows how it influences a large number of factors and cell receptors.
It has anti-hyperglycaemic activity. Berberine affects glucose metabolism by increasing insulin secretion (6) (which stimulates uptake of glucose by cells), by improving cellular insulin sensitivity and by stimulating glycolysis (the use of glucose) (7-8). In the small intestine, it also interferes with glycosidase, an enzyme responsible for transporting glucose across the intestinal epithelium. It’s likely, therefore, to slow down glucose absorption in the body (9).
It has anti-adipogenic activity. Although berberine reduces glycaemia, it does not increase fat cell volume. Research suggests it actually reduces the expression of several genes (by decreasing certain transcription factors) directly related to fatty tissue and adipogenesis (10).
It’s a powerful antioxidant. Recent studies have shown that free radical generation, associated with insulin-resistance, causes damage and large-scale suicide in beta-pancreatic cells (11-13). Oxidative stress also has a direct role in the development of the chronic complications of diabetes such as nephropathy, retinopathy and neuropathy (14). Berberine is also recognised for its ability to inhibit oxidation, particularly by upregulating several endogenous antioxidants such as superoxide dismutase (SOD) and glutathione, primarily in the liver (15-16). Its beneficial effect on oxidative stress has been observed in humans in a clinical trial: researchers noted a dramatic decrease in markers of oxidation after one month’s supplementation with berberine.
It’s an excellent anti-inflammatory. The role played by inflammation in the pathogenesis of diabetes is well documented (17). It’s known that numerous pro-inflammatory cytokines are involved in the development of insulin-resistance. Here again, berberine appears to offer benefits by reducing cytokine activity (18-20).
The story is the same if we look at human trials only. In some studies, berberine’s effects against diabetes have even been superior to those of commonly-used drugs (21), and with fewer side-effects (22). This recent research confirms that when taken orally, berberine is indeed bioavailable, contrary to what some scientists first thought. If concentrations of berberine in the blood are low following oral administration, it’s because it is rapidly transported to organs such as the liver and pancreas, where it’s metabolised into a number of active metabolites (23).
You only have to read the many reviews from those who decided to take berberine to be convinced of its quite remarkable efficacy. The following comments were made about the best-selling supplement Berberine 500 mg, a 100% natural product with unrivalled purity:
- « I’ve just placed my 3rd order (for 3 months’ supply) : effective from the outset at reducing blood glucose ... », Frédérique Lucas.
- « Amazingly effective! When my test results came back, my doctor got a fright », Jean Claude Escande.
- « We use berberine to reduce blood sugar levels and it works for us », Yolande Niquet.
- « I think it’s a fantastic product because it’s helped improve my type 2 diabetes whereas I got no benefit from all the conventional drugs and plenty of side effects, particularly hypoglycaemia », Annie Parlanti.
- « I recommend this product which I’ve been taking to replace an allopathic product which failed to solve the problem for years. After 3 months’ supplementation with Berberine, my test results showed improvements in every marker of glycaemia », Gaston Simon.
- « I’m over 75 and a type 2 diabetic. My doctor was amazed when I told him that thanks to berberine, my diabetes was in remission ».
- « I’ve been taking berberine for 3 years and along with a healthy diet and regular walking, it’s led to a considerable improvement in my diabetes. The doctors don’t want to admit it but when they see my test results, they have to agree. I’ve never experienced any side-effects, only benefits for my whole body, and no more urine infections. I thoroughly recommend this product », Sophie Dujardin.
For more customer reviews: avis sur la berbérine.
In fact, berberine is popular because its efficacy can be measured. As blood sugar levels are monitored regularly in diabetics, the effects of berberine can be quickly verified. Nobody can say « it’s all in your head » : this is a strictly objective assessment. It’s there in black and white in the test results.
5 tips to combat and reverse diabetes naturally
The study mentioned at the start of this article highlights the importance of losing weight in order to permanently reverse diabetes, but the participants involved were strictly controlled by the researchers. Without the benefit of such close supervision, how can you lose at least 10kg healthily and sustainably, and at the same time gradually lower your blood sugar levels? By drawing on the support of health professionals and natural aids and following some simple guidelines. Here are five essential tips for successfully reversing diabetes:
1) Start cooking (again) . This is the top tip for shedding abdominal fat: ditch the hyper-processed foods containing everything that’s bad for your diabetes: salt, saturated fats, hidden sugars (particularly fructose), sources of free radicals … Instead, prepare all your meals from scratch, prioritising vegetables, and you’ll go a long way to achieving your objective.
2) Support your efforts with berberine
3) Prioritise low GI foods. It’s now acknowledged that those suffering from diabetes benefit from considering the glycaemic index (GI) of the food they eat. A low GI diet leads to reduced blood glucose, healthier lipid levels and better weight control.
4) Learn to love fibre. Soluble fibre, which we’re eating less and less, is essential for anyone looking to reverse diabetes. It helps to slow down the absorption of glucose, get rid of excess weight and lower glycaemia. Diabetics are advised to consume between 25g and 50g of fibre a day from fruits and vegetables (turnips, asparagus, broccoli, cabbage, beans, onions, artichokes, oranges, peaches, pears, apples …) or from fibre supplements (psyllium taken with a glass of water at mealtimes is very effective: it reduces glucose and insulin levels by 10-20 % (24)).
5) Put your faith in antioxidants. The antioxidants found in all fruits and vegetables (especially brightly-coloured ones) are always worth prioritising. They’re essential for fighting numerous diseases and diabetes is no exception: the oxidative stress that occurs in this condition can lead to well-known complications such as atherosclerosis, kidney failure and retinopathy.
Study at the centre of this article:
Roy Taylor, Ahmad Al-Mrabeh, Sviatlana Zhyzhneuskaya, Carl Peters, Alison C. Barnes, Benjamin S. Aribisala, Kieren G. Hollingsworth, John C. Mathers, Naveed Sattar, Michael E.J. Lean. Remission of Human Type 2 Diabetes Requires Decrease in Liver and Pancreas Fat Content but Is Dependent upon Capacity for β Cell Recovery. Cell Metabolism, 2018; DOI: 10.1016/j.cmet.2018.07.003
References
 Berberine
BerberineBerberine HCL: natural extract of Berberis vulgaris for cardiovascular health
www.supersmart.comAll rights reserved
Free
Thank you for visiting our site. Before you go
REGISTER WITHClub SuperSmart
of exclusive benefits:
- Free: our weekly science-based newsletter "Nutranews"
- Special offers for club members only